Эпителиальные клетки (эпителии) в общем анализе мочи постоянно присутствуют в виде осадка мочи. Эпителиальных клеткок в моче двух видов: клетки плоского и переходного эпителия. Клетки плоского эпителия попадают в мочу из наружных половых органов и мочеиспускательного канала (уретры).
В моче у здорового человека эпителиальные клетки не должны обнаруживаються или обнаруживаются в единичных количествах в норме не более 3-ех в поле зрения. Выявление клеток почечного эпителия с цилиндрами в моче указывает о тяжелом поражении почек. При разнообразных поражениях мочеполовой системы присутствуют элементы почечного эпителия в моче , а также форменные компоненты крови — эритроциты и лейкоциты, а также мочевые цилиндры
Клетки плоского эпителия имеют полигональную или округлую форму, больших размеров, бесцветные, с небольшим ядром, располагаются в виде отдельных экземпляров или пластами.
Клетки переходного эпителия имеют различную величину и форму в зависимости от того, из какого отдела мочевыводящих путей происходят. Могут встречаться полигональные, «хвостатые», цилиндрические и округлые клетки, содержащие одно (довольно крупное) или несколько пузырьковидных округлых ядер; цитоплазма в большинстве заполнена каплями секрета и зернистостью. Окрашены они обычно в желтоватый цвет, интенсивность которого зависит от концентрации в моче пигментов (урохромов). Иногда в клетках наблюдаются дегенеративные изменения в виде грубой зернистости и вакуолизации цитоплазмы. Встречаются и двуядерные клетки. Клетки переходного эпителия могут встречаться в моче изолированно, скоплениями и в виде групп. Наличие групп и выявление в клетках признаков атипии требует проведения дифференциальной диагностики с элементами доброкачественных и злокачественных новообразований.
Клетки почечного эпителия и предстательной железы чрезвычайно схожи между собой. Они небольшого размера, неправильной круглой формы, угловатые или четырехугольные, с ядром, расположенным ближе к периферии цитоплазмы, слегка желтоватого цвета. Легко подвергаясь процессам дегенерации, клетки часто содержат зернышки белкового происхождения, вакуоли и жировые капли (в последнем случае значительно увеличиваются в размерах). В результате этих изменений ядра часто не выявляются.
При наличии гемоглобина или билирубина клетки этого эпителия могут окрашиваться в бурый и желтый цвет. Клетки почечного эпителия относятся к кубическому и призматическому эпителию, выстилающему почечные канальцы. Чаще они располагаются в виде групп или цепочек. В ряде случаев выявляются в виде комплексов округлой или фестончатой формы, состоящих из большого количества клеток различной величины с явлениями жирового перерождения.
Нормальные величины. В моче женщин, полученной без катетера, клетки плоского эпителия могут выявляться всегда. Кроме клеток поверхностного эпителия, в моче у женщин выявляется промежуточный и парабазальный плоский эпителий. Количественное взаимоотношение клеток плоского эпителия, исходящих из разных слоев, определяется фазой нормального цикла и периодами репродуктивной жизни женщины. В моче девочек выявляется промежуточный и парабазальный эпителий, в период полового созревания — промежуточный и поверхностный плоский.
В моче мужчин плоский эпителий обычно не встречается.
Клетки плоского и переходного эпителия встречаются обычно от единичных в препарате до единичных в поле зрения. Единичные в препарате клетки почечного эпителия на фоне нормальной микроскопической картины осадка мочи свидетельствуют о патологии.
Существенного диагностического значения клетки плоского эпителия не имеют, однако при их обнаружении расположенными пластами в осадке мочи, взятой катетером, необходимо исключить метаплазию слизистой оболочки мочевого пузыря, а также лейкоплакии мочевого пузыря и мочеточников, рассматриваемых как предопухолевые состояния.
Переходный эпителий выстилает слизистую оболочку мочевого пузыря, мочеточников, почечных лоханок, простатического отдела уретры и протоков предстательной железы.
Повышенная десквамация этих клеток наблюдается при остром и хроническом калькулезном цистите, пиелонефрите, почечнокаменной болезни, после инструментальных исследований (катетеризации, цистоскопии), приеме некоторых лекарственных препаратов (цитостатики, уротропин и др.).
Клетки почечного эпителия появляются в моче при поражениях:
- паренхимы почек при гломерулонефритах,
- пиелонефритах,
- нефропатии беременных,
- некоторых инфекционных заболеваниях,
- интоксикациях, расстройствах кровообращения.
Причины появления эпителиальных клеток в моче может быть разные, среди них:
- Воспаление мочевого пузыря, цистит в результате вирусной или бактериальной инфекции, поражение грибковой инфекцией.
- Нефропатия – болезни почек
- Нефропатия лекарственная, вызванная бесконтрольным применением некоторых лекарственных препаратов
- Различные уретриты
- Простатит
В любом случае появление незначительного количества эпителия в анализе мочи у женщин не должно вызывать тревогу, тогда как у мужчин это может свидетельствовать о уретрите.
источник
При микроскопическом исследовании в моче можно обнаружить клетки плоского, переходного и почечного эпителия, а также, изредка, раковые и атипичные клетки, которые могут указывать на развитие опухоли мочевого пузыря. Кроме этого, в отдельную группу выделяют пораженные вирусами decoy-клетки. Для плоского эпителия норма составляет 0-3 клетки в поле зрения, для почечного и переходного – единичные в препарате.
Случайное появление в моче эпителиальных клеток наблюдается очень часто. Оно не связано с патологическими процессами – болезнями или синдромами. Причиной их попадания в образец объясняется контактом мочи со стенками мочевыводящих путях, покрытыми эпителиальной тканью. Эпителиальные клетки живут относительно недолго, после чего замещаются новыми, а те, что отмирают, смываются мочой. Кроме того, одиночные клетки, составляющие отдельные ткани мочеполовой системы, также могут попадать в мочу вполне здорового человека.
С другой стороны, увеличение количества эпителиальных клеток в моче сверх нормы, должно вызывать беспокойство и рассматриваться вместе с другими показателями общего клинического анализа мочи с целью выявления возможного заболевания. Появление в моче клеток тканей почек и раковых клеток, всегда должно быть поводом для дальнейших исследований. Довольно часто в анализе количество обнаруженных клеток указывается не в единицах на поле зрения, а в полуколичественных терминах: одиночные, несколько, среднее количество и много.
Виды эпителиальных клеток в моче
Эпителиальные клетки составляют одну из четырех основных типов тканей, включающих также соединительную, мышечную и нервную ткани. Эпителиальные ткани обычно покрывают полости и поверхности кровеносных сосудов и органов по всему телу, включая слизистые оболочки и урогенитальные пути. Обычно рассматривают три основных типа эпителиальных клеток, которые можно найти в моче. Их вид, количество и пропорция могут помочь врачам выяснить, откуда они появились, и, возможно, почему они обнаружены в моче.
Плоский (прямоугольный) эпителий. Эти клетки типичны для поверхности мочеиспускательного канала (уретры). Их появление в моче преимущественно является следствием загрязнения образца при неправильном сборе и несоблюдении гигиены. Впрочем, наличие большого количества плоского эпителия, при условии надлежащего сбора мочи, может указывать на вероятный вагинит или уретрит, поскольку воспалительный процесс поражает стенки мочеиспускательного канала, которые выстеляются именно плоским эпителием. Также, при подсчете, иногда обнаруживают подвид плоского эпителия, известный под названием clue cells – это плоскоклеточные эпителиальные клетки с бактериями Gardnerella vaginalis, которые колонизируют клетку. Их выявление является признаком бактериального вагиноза.
Переходный эпителий. Этот тип эпителиальных клеток характерен для тканей почечной лоханки, мочеточников, проксимальной части мочеиспускательного канала и мочевого пузыря. Воспалительные процессы, вызванные инфекцией перечисленных органов, могут привести к появлению большого количества переходного эпителия в моче. Некоторыми исследованиями показано, что у мужчин с хламидийными уретрит (возбудитель – хламидия C. trachomatis) в моче появляется значительное количество переходных эпителиальных клеток. Сферическая форма переходного эпителия является проблемой при дифференциации его с почечным канальцевым эпителием. Для надежного подсчета переходного эпителия рекомендуют его окрашивать.
Почечный эпителий. Представляет собой канальцевые (тубулярные) клетки почек, являющиеся частью нефронов и играющие важную роль в реабсорбции воды и солей. Почечный эпителий обычно не появляется в моче здорового человека. Таким образом, их присутствие практически всегда связано с повреждением почек, такими как острый канальцевый (тубулярный) некроз, вирусные заболевания (например, цитомегаловирусный нефрит), пиелонефрит и токсические реакции на некоторые вещества. Клетки почечного эпителия могут поглощать пигменты, такие как билирубин, или содержать вакуоли (если вакуоли не содержат липидов – их называют пузырчатыми клетками или bubble cells, если же наполнены жиром, то овальными жировыми телами).
Нефротический синдром – это распространенное поражение почек, которое характеризуется повреждением их тканей и существенным ростом количества белка в моче, или протеинурией. Появление значительного количества белка является следствием поражения нефронов – клеточных элементов почек, отвечающих за фильтрацию крови и образование мочи. При ощутимом поражении нефронов в моче появляются канальцевые (тубулярные) клетки, которые являются важным элементом нефронов. Их выявление в моче помогает врачам подтвердить факт развития у пациента нефротического синдрома.
Decoy-клетки – эпителиальные клетки мочи, инфицированных вирусами. Их название (decoy переводится как призрак, ловушка, приманка) связано с их похожестью на раковые клетки, которые также обнаруживаются в моче. Таким образом, decoy-клетки могут привести к ложному диагностированию рака мочевого пузыря у здорового пациента. Они распространены у пациентов с низким иммунитетом, например, у больных, перенесших трансплантацию и получают иммуносупрессивные лекарства для предотвращения отторжения. У пациентов, перенесших трансплантацию почек, эти клетки обнаруживают в 40% случаев. Несколько типов вирусов могут косвенно влиять на появление этих клеток, в том числе цитомегаловирус и полиомавирус (polyomavirus). В некоторых случаях выявление decoy-клеток является значимым для врачей при диагностике клинических состояний, таких как полимомавирусная нефропатия (после трансплантации почки) или геморрагический цистит (после трансплантации гемопоэтических стволовых клеток).
Клетки опухолей – атипичные клетки, которые обнаруживают в моче. Совместные исследования специалистов различного профиля показали важную роль исследования раковых клеток в выявлении карциномы высокой степени злокачественности: как тех, что выявлении впервые, так и тех, которые уже наблюдаются. Важным преимуществом этого метода является доступность материала, легкость его получения; он не предусматривает хирургического вмешательства. При этом в отношении уротелиальних карцином чувствительность метода составляет 80-90%, а специфичность — 90-99%.
Согласно рекомендаций Европейской ассоциации урологов (European Association of Urology) разработана схема оценки результатов исследования цитологических мазков из мочи. В ней имеются 7 категорий: от негативной цитограммы до уротелиальной карциномы высокой степени злокачественности (HGUC) и других опухолей (первичных и вторичных):
источник
Epithelial cells are a type of cell that lines the surfaces of your body. They are found on your skin, blood vessels, urinary tract, and organs. An epithelial cells in urine test looks at urine under a microscope to see if the number of your epithelial cells is in the normal range. It’s normal to have a small amount of epithelial cells in your urine. A large amount may indicate an infection, kidney disease, or other serious medical condition.
Other names: microscopic urine analysis, microscopic examination of urine, urine test, urine analysis, UA
An epithelial cells in urine test is a part of a urinalysis, a test that measures different substances in your urine. A urinalysis may include a visual examination of your urine sample, tests for certain chemicals, and an examination of urine cells under a microscope. An epithelial cells in urine test is part of a microscopic exam of urine.
Your health care provider may have ordered an epithelial cells in urine test as part of your regular checkup or if your visual or chemical urine tests showed abnormal results. You may also need this test if you have symptoms of a urinary or kidney disorder. These symptoms may include:
Your health care provider will need to collect a sample of your urine. During your office visit, you will receive a container to collect the urine and special instructions to make sure that the sample is sterile. These instructions are often called the «clean catch method.» The clean catch method includes the following steps:
- Wash your hands.
- Clean your genital area with a cleansing pad given to you by your provider. Men should wipe the tip of their penis. Women should open their labia and clean from front to back.
- Start to urinate into the toilet.
- Move the collection container under your urine stream.
- Collect at least an ounce or two of urine into the container. The container will have markings to indicate the amounts.
- Finish urinating into the toilet.
- Return the sample container as instructed by your health care provider.
You don’t need any special preparations for the test. If your health care provider has ordered other urine or blood tests, you may need to fast (not eat or drink) for several hours before the test. Your health care provider will let you know if there are any special instructions to follow.
There is no known risk to having the test.
Results are often reported as an approximate amount, such as «few,» moderate,» or «many» cells. «Few» cells are generally considered in the normal range. «Moderate» or «many» cells may indicate a medical condition such as:
If your results are not in the normal range, it doesn’t necessarily mean that you have a medical condition that requires treatment. You may need more tests before you can get a diagnosis. To learn what your results mean, talk to your health care provider.
There are three types of epithelial cells that line the urinary tract. They are called transitional cells, renal tubular cells, and squamous cells. If there are squamous epithelial cells in your urine, it may mean your sample was contaminated. This means that the sample contains cells from the urethra (in men) or the vaginal opening (in women). It can happen if you do not clean well enough when using the clean catch method.
- Ask a Biologist [Internet]. Tempe (AZ): Arizona State University: School of Life Sciences; c2016. Viral Attack: Epithelial Cell [cited 2017 Feb 12]; [about 4 screens]. Available from: https://askabiologist.asu.edu/epithelial-cells
- Hinkle J, Cheever K. Brunner & Suddarth’s Handbook of Laboratory and Diagnostic Tests. 2 nd Ed, Kindle. Philadelphia: Wolters Kluwer Health, Lippincott Williams & Wilkins; c2014. Urinalysis; 509 p.
- Johns Hopkins Lupus Center [Internet]. Johns Hopkins Medicine; c2017. Urinalysis [cited 2017 Feb 12]; [about 4 screens]. Available from: https://www.hopkinslupus.org/lupus-tests/screening-laboratory-tests/urinalysis/
- Lab Tests Online [Internet]. American Association for Clinical Chemistry; c2001–2017. Urinalysis: The Test [updated 2016 May 26; cited 2017 Feb 12]; [about 4 screens]. Available from: https://labtestsonline.org/understanding/analytes/urinalysis/tab/test
- Lab Tests Online [Internet]. American Association for Clinical Chemistry; c2001–2017. Urinalysis: The Test Sample [updated 2016 May 26; cited 2017 Feb 12]; [about 3 screens]. Available from: https://labtestsonline.org/understanding/analytes/urinalysis/tab/sample/
- Lab Tests Online [Internet]. American Association for Clinical Chemistry; c2001–2017. Urinalysis: Three Types of Examinations [cited 2017 Feb 12]; [about 2 screens]. Available from: https://labtestsonline.org/understanding/analytes/urinalysis/ui-exams/start/2/
- Mayo Clinic [Internet]. Mayo Foundation for Medical Education and Research; c1998–2017. Urinalysis: How you prepare; 2016 Oct 9 [cited 2017 Feb 12]; [about 3 screens]. Available from: http://www.mayoclinic.org/tests-procedures/urinalysis/details/how-you-prepare/ppc-20255388
- Merck Manual Consumer Version [Internet]. Kenilworth (NJ): Merck & Co., Inc.; c2016. Urinalysis [cited 2017 Feb 12]; [about 2 screens]. Available from: https://www.merckmanuals.com/home/k >
The medical information provided is for informational purposes only, and is not to be used as a substitute for professional medical advice, diagnosis or treatment. Please contact your health care provider with questions you may have regarding medical conditions or the interpretation of test results.
In the event of a medical emergency, call 911 immediately.
источник
Epithelial cells are cells that come from surfaces of your body, such as your skin, blood vessels, urinary tract, or organs. They serve as a barrier between the inside and outside of your body, and protect it from viruses.
A small number of epithelial cells in your urine is normal. A large number may be a sign of infection, kidney disease, or another serious medical condition. For that reason, your doctor may order a urine test or urinalysis to view your urine under a microscope.
Epithelial cells differ by size, shape, and appearance. There are three types of epithelial cells that can be found in your urine, depending on their origin:
- Renal tubular. These are the most important of the epithelial cells. An increased number can mean a k >
A urine test may show that you have “few,” “moderate,” or “many” epithelial cells in your urine.
Epithelial cells naturally slough off from your body. It’s normal to have one to five squamous epithelial cells per high power field (HPF) in your urine. Having a moderate number or many cells may indicate:
The type of epithelial cells in the urine may also signal certain conditions. For instance, epithelial cells that contain a large amount of hemoglobin, or blood particles, may mean that you recently had red blood cells or hemoglobin in the urine, even if they weren’t there during the urinalysis.
More than 15 renal tubular epithelial cells per HPF may mean your kidney isn’t working properly.
Squamous epithelial cells in your urine may just mean the sample is contaminated.
A urinalysis that finds squamous epithelial cells in the urine isn’t the norm, William Winter, MD, a clinical chemist for Shands Hospital and professor of pathology and pediatrics at the University of Florida, told Healthline.
That’s because the clean catch method of obtaining a urine sample usually prevents squamous epithelial cells from turning up in the urine. When using the clean catch technique, you’ll be given a sterilizing cloth to wipe the area around the vagina or penis before giving your urine sample. This prevents contaminants from your skin, like epithelial cells, from showing up in your sample.
Your doctor can help you understand your test results and whether you have a medical condition requiring treatment. To find a cause, the doctor may also order further testing.
You may be at increased risk for high counts of epithelial cells if you:
Treatment will depend on the cause of the abnormal number of epithelial cells. Most UTIs are bacterial and can be treated with an antibiotic. Drinking more water can also speed healing. For viral UTIs, doctors may prescribe medication called antivirals.
Treatment for kidney disease means managing the underlying cause of the disease, including blood pressure, blood sugar, and cholesterol levels. Your doctor may prescribe a blood pressure medication to slow the progression of the disease or preserve kidney function, even if you don’t have high blood pressure. Healthy dietary and lifestyle changes are also important.
Your doctor may advise you to:
- control diabetes through insulin injections
- cut back on foods high in cholesterol
- cut back on salt
- increase physical activity
- limit alcohol
- lose weight
- start a heart-healthy diet that includes fresh fruits, vegetables, and whole grains
- quit smoking
источник
Squamous epithelial cells are usually found in very small numbers in a urine sample. When looking for a urinary tract infection, doctors have to examine the type of epithelial cells that are in the urine. The presence of a large number of epithelial cells in a urinalysis test may indicate a bacterial infection, however, having many squamous epithelial cells (SECs) in urine usually indicates that the urine sample was contaminated.
There are three types of epithelial cells that can show up in urine. According to doctors from the Mayo Clinic, the 3 types of epithelial cells are: 1
- Squamous epithelial cells
- Transitional epithelial cells
- Renal epithelial cells
Transitional epithelial cells are found in the uterus and bladder. As their name would suggest, renal epithelial cells are found in the kidneys. According to Johns Hopkins, the finding of renal epithelial cells in urine may indicate a problem with the kidneys. 2
This article looks in depth at squamous epithelial cells and what their presence in a urine sample indicates. We will also examine if squamous epithelial cells could be a sign of a urinary tract infection (UTI).
Squamous epithelial cells are found in your urinary tract and are described as flat skin cells with an irregular outline. According to the Mayo Clinic, squamous epithelial cells are large epithelial cells with up to 5 nuclei. 1
Although many websites say that the presence of squamous epithelial cells indicates a kidney disease, this is not the case. The Faculty of Medicine in Masaryk University says that squamous epithelial cells originate from the urethra or vagina and are commonly found in urine samples. However, it’s the presence of transitional epithelial cells that would indicate a urinary tract infection. Or, if a large number of renal epithelial cells are discovered in urinalysis, then it could indicate a viral infection or problem with your kidneys. 3
If your urine sample shows many squamous epithelial cells, what does that mean? Should you be worried about squamous epithelial cells in urine?
According to Dr. Edgar Lerma on Medscape, the normal range of squamous epithelial cells in urine is up to 15-20 squamous epithelial cells/hpf. However, a reading of more than 15-20 SEC/hpf usually indicates that the urine specimen has been contaminated and a new sample should be taken. 4
Doctors carry our urine analysis to look for the presence of bacteria and germs which cause infection or disease. In fact, the absence of squamous cell from a urine sample can still be an indicator of a UTI.
Dr. Edgar Lerma on Medscape says that urinalysis checks for nitrites in the urine and leukocytes (white blood cells) in urine as well as bacteria. If bacteria are found in the urine but no squamous cells, that could be a strong indicator of a UTI. 4 In fact, the journal Academic Emergency Medicine reports that the presence of a few squamous epithelial cells can better help to identify bacteria in urine samples. However, the report states that even a large number of SECs doesn’t always indicate a contaminated urine sample. 5
The number of SECs, as well as the presence of other chemicals in the urine, can also help rule out UTIs. If there are a low number of squamous epithelial cells and there are no nitrates or pus in the urinalysis, then urinary tract infections can be ruled out. 5
When a doctor asks you to take a urine sample, they will look for certain indicators as to your general health. Dr. Adam Husney on WebMD says that there is a lot that the color of your urine can tell about your health. 6 Also, the level of nitrites in your urine can indicate the presence of bacteria. If you have white blood cells in your urine, that could indicate an infection in your urinary tract or inflammation in your bladder.
Other factors in your urine sample that can help doctors identify specific health issues are:
- Clarity. Urine should be a pale-yellow color that isn’t cloudy.
- Odor. There should be no strong smell from your urine.
- pH level. Keeping the pH levels of your urine balanced can help prevent kidney stones from forming.
- Glucose. Blood sugar levels can indicate the presence or risk of diabetes.
- Protein. Your urine should not contain protein.
If you must collect a urine sample, your doctor will usually give you an appropriate container to collect the urine sample. Dr. Husney says that if you need to make yourself pee to collect a sample, you should avoid consuming foods like beets or blackberries to avoid coloring your urine.
It’s also important to avoid contaminating the urine sample with bacteria as this could cause a large number of squamous epithelial cells to show up in the urinalysis. So, it’s important to always wash your hands before and after collecting a sample. Women should clean the area around the urethra by wiping from front to back. You should also collect the urine sample mid-flow without stopping. After you have enough urine in the container, finish peeing in the toilet then close the container tightly.
Dr. Gary David Steinberg says that squamous cell carcinoma is a type of bladder cancer. Usually, doctors will carry out a urine test to check for blood in urine. Doctors may also include a urine culture in the tests to check for infection and the presence of cancer. 7
However, blood in the urine can also be a sign of a urinary tract infection or bladder infection.
Although the presence of squamous epithelial cells in urine isn’t by itself a sign of a UTI, many people assume that this is the case. If you think that you have a urinary tract infection, what can you do to resolve it?
Here are some natural remedies to help treat a urinary tract infection naturally:
Drinking baking soda water can help you reduce the painful symptoms of a UTI because it neutralizes acid in urine. The Cochrane Library reported that sodium bicarbonate (baking soda) helps to alkalize urine and can help reduce recurrent UTIs in women. 8
All you have to do is mix ½ to 1 teaspoon of baking soda in a glass of water and drink on an empty stomach. Drink the baking soda remedy 2-3 times a day. If your symptoms persist after 2 days, you should visit your doctor.
Raw, plain yogurt contains probiotics and can help take the sting out of a UTI and help reduce vaginal itching and discomfort. The journal Drugs stated that probiotics help to increase “good bacteria” in the vaginal area and help to prevent urinary tract infections. 9
You can coat a tampon in raw yogurt and place this inside your vagina. Apply the yogurt tampon 3-4 times a day to help relieve the symptoms of urinary tract infection. Also consume a few large spoons of raw yogurt several times a day to help increase “good” bacteria in your digestive and urinary tract.
You can also take probiotic supplements. The University of Maryland Medical Center says that the best-known probiotics for treating UTI are the lactobacilli strains, such as acidophilus, which is found in yogurt and kefir, as well as in dietary supplements. 12
Vitamin C is a good all-around vitamin that helps boost your immune system and it also has a positive effect in treating urinary tract infection. Taking vitamin C when the first sign of UTI appears can help prevent the infection from getting worse. This is why raw cranberry juice is a common remedy for UTI as it contains a large amount of vitamin C and anti-oxidants that contribute to healthy bladder function.
Various studies also confirm using vitamin C for treating UTI, for example: The journal Urology reported that vitamin C may be an effective treatment for bacteria in urine. 10 Johns Hopkins Medicine reports that treating a urinary infection with large amounts of vitamin C limits the growth of some bacteria and vitamin C supplements can help to do this. 11
According to the University of Maryland Medical Center, taking 500 to 1,000 mg of vitamin C, 1 to 2 times daily may be beneficial for managing bladder infections and for immune support. 12
You can find other ways to treat UTI in my article on how to treat urinary tract infection (UTI) naturally, such as D-Mannose, bromelain, cranberry juice and apple cider vinegar (ACV).
источник
Squamous epithelium is a normal finding in the dorsal trachea near the junction between the membranous and cartilaginous portion of the trachea.
Donald B. McMillan, Richard J. Harris, in An Atlas of Comparative Vertebrate Histology , 2018
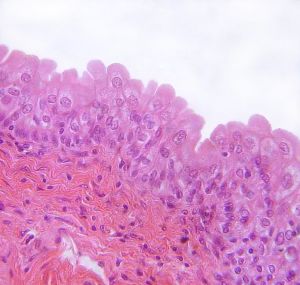
Squamous epithelial cells . The form and appearance of isolated squamous cells can be observed in desquamated cells from the superficial layer of the lining of the mouth ( Figs. C6a and C6b ). In the preparation shown here, little detail is obtained using an ordinary bright field microscope ( Fig. C6a ); the use of differential interference contrast (DIC) ( Fig. C6b ) enhances the image. Note the thin, scale-like appearance of the cells, their nuclei, cytoplasm, cell membrane, and the relative size and location of the nuclei. Fig. C7 is a whole mount of the layer of flattened cells that constitutes the peritoneal lining of the coelom. The tissue is composed of flat, polygonal cells fitted closely together in the manner of a pan-full of fried eggs; in this preparation, the intercellular cement has been blackened with a silver precipitate and the nuclei are stained pale violet. In Fig. C8 these cells are shown in a section of this tissue. Fig. C9 shows squamous cells as they appear in a section of the nephric capsule of the kidney. The “fried eggs” may be rolled up to form tubes—blood capillaries—that constitute the smallest components of the vascular system; exchange of nutrients and wastes occurs across these thin cells ( Figs. C10a and C10b ).
Figure C6a . Little detail is seen with the ordinary bright field microscope.
Figure C6b . Detail is enhanced by the use of differential interference microscopy.
Figure C6 . Fresh squamous epithelial cells scraped from the inside of the human cheek. 63×.
Figure C7 . This is a surface view of the peritoneum that lines the body cavity of a vertebrate. The cementing substance between individual cells is stained black with silver. Like a pan of fried eggs, mutual pressure of the cells of this simple squamous epithelium causes them to assume a roughly hexagonal shape. The faint violet nuclei of some of the cells may be discerned. 40×.
Figure C8 . The “fried eggs” of a simple squamous epithelium are sliced and seen in side view at the right this section of the peritoneum of a mammal. They rest on vascular connective tissue. 63×.
Figure C9 . A simple squamous epithelium lines the urinary space in the kidney of a frog. Most of the micrograph is occupied by sections through tubules of the kidney. 40×.
Figure C10a . Simple “fried eggs” may be rolled up to form a thin-walled tube, as in this whole mount of the skin of Ambystoma showing a thin-walled blood vessel, a CAPILLARY containing oval nucleated blood cells. 100×.
Figure C10b . A cross section of a capillary, looking much like a signet ring, is at the center is of this section of the foot of a toad. Most of the section is occupied by cross sections of muscle cells. Several other sectioned capillaries are scattered throughout. 63×.
Cuboidal epithelial cells. In this section of the thyroid gland, note the shape of the cells forming the follicles as well as the shape and position of the nuclei ( Fig. C11 ).
Figure C11 . A simple cuboidal epithelium surrounds yellowish colloidal material in follicles of the thyroid gland of a mammal. Often cell membranes are not visible in sections. If you imagine cell membranes between each pair of nuclei, the cells become simple cuboidal in your mind. 100×.
Columnar epithelial cells. Columnar epithelial cells range from those whose height is only slightly greater than their other two dimensions to those that are greatly elongated. The nuclei are usually found toward the base. Identify the columnar epithelium in sections of vertebrate gallbladder and intestine ( Figs. C12 and C13 ). Note the shape and location of the nuclei.
Figure C12 . The gallbladder of a toad is lined with a simple columnar epithelium . 100×.
Figure C13 . An absorptive simple , columnar epithelium lines the intestine of a cat. Note the two cells at the left that resemble stemmed goblets; they secrete mucus. 63×.
E. Laura Munteanu, . Nicolas Biais, in Methods in Cell Biology , 2015
A431 epithelial cells, squamous carcinoma line. Other cell lines with medical relevance in respect to infections could be used. We use epithelial cells as Ng infects epithelia.
MS11-mCherry Kan, wild-type Ng that constitutively expresses cytoplasmic mCherry. The strain is resistant to kanamycin.
DMEM (Himedia AL007S-500 ML);
Fetal bovine serum (FBS) (CORNING cellgro-500ML, VWR 45000-734);
Trypsin (Gibco TrypLE, Life Technologies 12604-013);
Fiber tipped applicator (sterile Dacron swabs) (VWR 22222-046);
1.5 mL microcentrifuge tubes (Neptune, VWR 89134-506) ;
15 mL centrifuge tubes (VWR 89039-664) ;
Cell culture petri dishes 100 × 20 mm, treated, sterile (CORNING 430167);
Six-well plates 5 mL, sterile (VWR 29442-042);
Round 25 mm Ø microscope coverslips (Warner Instruments 64–0705);
Teflon coverslip racks (Life Technologies);
AttoFluor cell chamber (Molecular Probes A7816) ( Figure 2(A) );
Bauer hemocytometer (Amazon);
CoolCell freezing box (VWR 95059-860).
Sterile hood (BSL2 Biosafety);
Cell incubator at 37 °C and 5% CO2;
The PVs have a specific tropism for squamous epithelial cells (keratinocytes). The functions of the PVs necessary for production of infectious virions, which include vegetative viral DNA replication and the synthesis of the capsid proteins, occur only in the fully differentiated squamous epithelial cells of a papilloma. Viral DNA replication for progeny virion production can be detected by in situ hybridization only in the more differentiated squamous epithelial cells of the stratum spinosum and of the granular layer of the epidermis, but not in the basal layer nor in the underlying dermal fibroblasts. Viral capsid protein synthesis and virion assembly occur only in the terminally differentiated cells of the upper layers of the epithelium. The viral genome is present in the epithelial cells of all layers of the epithelium, including the basal layer. It is generally believed that the expression of specific viral genes in the basal layer and in the lower layers of the epidermis stimulates cellular proliferation and alters the keratinocyte differentiation profile, characteristics of a wart. As squamous epithelial cells migrate upward through the layers, they undergo a program of differentiation. The control of papillomavirus late-gene expression is tightly linked to the differentiation state of the squamous epithelial cells. The basis of this control is not yet fully understood, but involves the activation of a “late” promoter and altered patterns of viral messenger RNA processing ( 13 ).
The genomic organization of all the PVs is quite similar. All of the open reading frames (ORFs) that could serve to encode proteins for these viruses are located on only one of the two viral DNA strands and only one strand is transcribed. The HPV genome can be divided into three distinct regions: (1) an “early” region that encodes the viral proteins (E1, E2, etc.) involved in viral DNA replication, transcriptional regulation, and cellular transformation; (2) a “late” region that encodes the viral major (L1) and minor (L2) capsid proteins; and (3) a region called the long control region (LCR) or alternatively, the upstream regulatory region (URR), which does not contain any ORFs, but does contain cis-regulatory elements, including the origin of DNA replication and important transcriptional enhancers. A diagram of the organization of the HPV-16 genome, which is typical of all the HPVs, is shown in Figure 6-2 . In productive infections (i.e., infections in which viral particles), messenger RNA is transcribed from the early and late regions of the genome. However, the late genes (L1 and L2) are only expressed in the more differentiated cells of the epithelium. The nonproductive phase of the infectious cycle occurs in the less differentiated cells in the lower epithelium and is accompanied by expression of the early (E) region genes.
Figure 6-2 . M ap of the HPV-16 genome. The nucleotide numbers are noted within the circular maps, transcription proceeds clockwise, and the major open reading frames (E1 to E7, L1, and L2) are indicated. The transcriptional promoter that directs the expression of E6 and E7 is designated (P97). AE and AL represent the polyadenylation signals for the early and late transcripts, respectively. The viral long control region (LCR) contains the viral transcriptional and replication regulatory elements. The closed circles on the genome represent the four E2 binding sites that have been noted in the LCR.
источник
The presence of squamous epithelial cells in a urine sample is often an indication that the sample has been contaminated, according to the John Hopkins Lupus Center.
However, epithelial cells can also indicate urogenital problems, including infections, inflammation and malignancies, as Lab Tests Online explains. Typically, doctors report the extent of squamous epithelial cells in a urine specimen as few, moderate or many, based on microscopic examination. The term «few» refers to a normal range while «moderate» and «many» can mean the presence of a medical condition.
What are Squamous Epithelial Cells?
Squamous epithelial cells occur in many different parts of the body and serve to cover a given structure or cavity. Although they are often thought of as skin cells, they can actually be found covering many layers of the human body, both inside and out. For example, squamous cells are found in the mouth, cervix and middle skin layers.
Squamous epithelial cells are flat and thin as opposed to cube-shaped. They are the thinnest type of epithelial cell and have a large surface area. Their shape allows for molecules to move across their membrane easily, making them useful for filtration and diffusion.
How is a Microscopic Examination Performed?
Microscopic urinalysis involves centrifuging a test tube of urine to separate the components. The supernatant, or top layer, is discarded. The urine sediment and remaining urine are then analyzed using a microscope under low-power. This identifies squamous cells, crystals and casts. Then the sample is further analyzed at high power to identify bacteria, additional cells like red and white blood cells or clumps of cells.
What Other Types of Epithelial Cells are Found in Urinalysis?
There are three types lining the urinary tract. As well as squamous cells, there are also renal tubular cells and transitional cells. Determining the type of epithelial cells present in a urine sample can help the doctor determine whether the cells are originating from the bladder, urethra, kidneys or elsewhere, points out Lab Tests Online. Renal tubular cells are found in the kidneys while transitional cells are found in the bladder and uterus.
Is a Certain Level of Squamous Epithelial Cells in Urine Considered Normal?
The absence of any squamous epithelial cells in urine could possibly indicate a urinary tract infection. Generally speaking, a sample of 15 to 20 squamous epithelial cells/hpf is considered to be normal. Anything above that indicates that the sample may be contaminated. If that’s the case, the doctor will request a new sample.
Apart from Contamination, What Else Can High Levels of Squamous Cells Indicate?
If an abundance of cells is found in another, fresh sample, it could indicate a urinary tract infection. Other medical conditions as a result of moderate or many cells could be a yeast infection, kidney disease and liver disease. Squamous epithelial cells can also be linked to types of cancer. Squamous cell carcinoma is the most common type of oral cavity cancer and the second most common type of skin cancer. The latter type spreads to other parts of the body but is treated easily when caught early enough.
If moderate or many squamous cells are found, the doctor will carry out additional tests and evaluate the patient’s symptoms to ascertain if a medical condition is present and what measures can be taken to rectify it.
источник
Last Updated on November 25, 2019
While pregnant, you will have to take certain tests to ensure that your baby is developing fine and that you are healthy too. Your doctor might suggest a urine test to check for epithelial cells in your urine. They are found on the skin, vessels, urinary tract, and organs. While it is normal to have a few epithelial cells in the urine, a large number can indicate several problems and can be a cause of concern. A large number of cells can be a sign of urinary tract infection, yeast infection, kidney disease, liver disease and certain types of cancer. If you are pregnant, read on to learn about epithelial cells, their normal range in the urine during pregnancy, and more.
Epithelial cells line the surfaces of our body, such as the skin, inside of the throat, intestines, all the organs and blood vessels. They are tightly packed and function as a barrier between the inside and outside of the body, protecting it from the virus. However, sometimes viruses can find places to get through the epithelial cells to further invade the body and cause disease. Since epithelial cells make up the first layer of tissue on the organs they are present in different forms and sizes to perform different functions wherever they are present. Epithelial cells even line the inside of your food pipe and intestine where they help in the digestion and absorption of food that you eat. In other areas, they secrete enzymes, hormones and mucus in the body.
Epithelial cells vary in their shape, size and appearance. Majorly, there are three types that can be found in the urine sample.
These cells originate from the tissues that lie anywhere between the urethra and renal pelvis. They are able to stretch readily to accommodate changes in the volume of liquids in an organ.
These are large epithelial cells and originate from the female vagina and urethra. Squamous epithelial cells are the most commonly seen cells in urine during pregnancy.
The renal tubular epithelial cells are from the kidneys and an increased number of these cells can be a sign of a kidney disorder.
In order to understand the number of epithelial cells, you will need to undergo a urine evaluation test. The technician will look for the number of visible cells in a High Power Field (HPF) under a microscope. Based on how many they see, the tests report will indicate few, moderate or many numbers of epithelial cells. Since these cells are shed from the body as an ongoing build and repair process, the normal range of epithelial cells in urine during pregnancy or prior to it can range from 1 to 5 flat cells under high power field.
Pregnant women generally have a slightly higher count of epithelial cells in the urine as their bodies are going through a lot of changes, therefore even 8-10 epithelial cells in urine should not be alarming during pregnancy. However, further tests to look for urinary tract infection, yeast infection or inflammation caused by another condition should be carried out. Higher ranges of epithelial cells than these are a cause of concern, for example, more and 15 renal tubular epithelial under high power field indicates a problem in the kidneys.
If it is found that you have 15-20 epithelial cells in your urine during pregnancy or more, you need to worry. Technicians have to first rule out the possibility of the presence of large amounts of sediments in the first urine sample that may be concentrated. It means you will have to drink more water and go for another urine test after some time. If there are significant epithelial cells in the subsequent testing, it could be because of one of the following causes:
It is completely normal to lose some epithelial cells on a regular basis. All the organs in your excretory system have epithelial cells and they are shed now and then as part of the body’s ongoing repair and maintenance. If you drink less fluids before a test and the urine is concentrated, it is possible to get a sample with high epithelial cells. 2. Contamination
It is easy to contaminate the sample collecting cup if you do not follow the proper procedure to collect urine. If your genital is not clean prior to the test, it could contaminate the sample as there would be an accumulation of epithelial cells which would pass into the sample container. The same could happen if you fail to properly use the cleaning wipes provided to you to clean your genitals. Sometimes the cup can get contaminated when you touch its interior or it may have contaminants from the start, these could also throw off the readings. If you have suspicions of any of these, ask for another cup for a fresh sample to clear all doubts.
Urinary tract infections generally begin at the urethra from where the bacteria proliferate upward into the urinary system such as the bladder and finally the kidneys. When the bladder lining is irritated or inflamed, it causes sloughing of the epithelial cells in the bladder which can be found in the urine sample. In a severe UTI case which has made its way to the kidneys, it is possible to find renal epithelial cells in the urine samples and the doctor would treat the infection accordingly. It is important to note however that there could be other serious causes which can lead to similar test results as a UTI and as such, your doctor would look into it carefully. When random urine samples come back with high epithelial cells, UTIs must be ruled out first before proceeding further.
Pathologists also look for a particular type of cells coming from the kidneys. Finding epithelial cells from the renal tubes could indicate a severe infection in the kidneys or other kidney issues. The renal tubes function to filter out blood and produce urine. Finding a large number of these cells in a urine sample could be an indication of nephrotic syndrome. This condition is always caused by damage to the kidneys.
Treatment that follows the test depends on the cause of the abnormal numbers of epithelial cells and their types. Most of the UTIs are caused by bacteria and hence treated with antibiotics. The viral UTIs are treated with antivirals. Kidney disease is treated by managing the underlying cause such as high blood pressure, high cholesterol, and blood sugar levels. Your doctor may also advise you on the following:
- Healthy dietary changes
- Cutting back on high-salt and high-cholesterol foods
- Blood pressure medication to manage the progression of the disease and preserve kidney function
- Drinking plenty of water to stay well hydrated
- Cranberry juice to ward of UTIs
Finding epithelial cells in urinalysis is generally not a cause for alarm. Further testing and confirmation can rule out other variables and establish a cause. If you have a large number of epithelial cells in your urine, consult your doctor – she will guide you the best. Take precautionary measures and have a healthy pregnancy!
источник
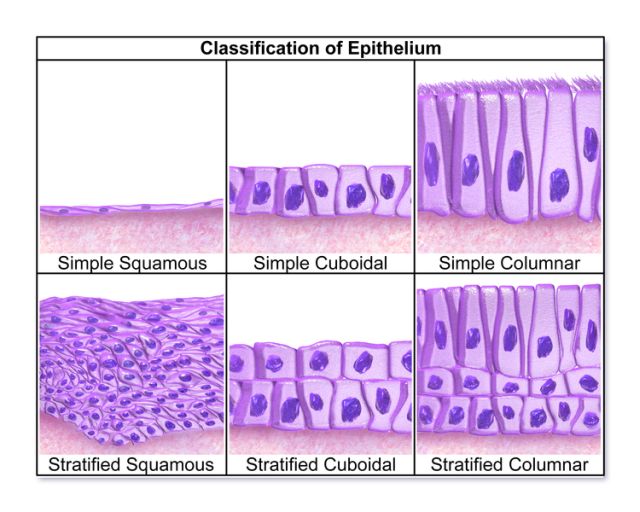
„Classification of Epithelium“ by Blausen.com staff. “Blausen gallery 2014“. Wikiversity Journal of Medicine 1 (2). doi:10.15347/wjm/2014.010. ISSN 20018762 .
The epithelium is a complex of specialized cellular organizations arranged into sheets without significant intercellular substance. They always occupy boundary surfaces of the body, i.e., they are located on the skin surface or on the internal surface of hollow organs. From an embryological perspective, epithelial tissue derives from all three germ layers. Depending on their function, epithelial cells can be flat, cuboidal or cylindrical and are organized in either one or several layers. Epithelial cells connect to two different spaces and thus have an apical and a basal pole.
Apical derives from the term apex which means peak. Basal, on the other hand, derives from the base. In the medical nomenclature for hollow organs, the term luminal is often used to refer to the pole which faces the lumen. The pole oriented away from the lumen is called abluminal. The cell’s sidewalls are often structurally and functionally correspondent to the base and are referred to as a basolateral membrane. In other parts, epithelial tissues are forming the inner lining and external lining of body parts. To summarize, the apical pole faces the surface, while the basal pole is attached to the connective tissue located below the epithelium.
There are three different types of epithelial tissue: squamous, cuboidal, and columnar. The differentiation and classification of the types of epithelial tissue are based on the shape of the cell (e.g., cuboidal), the arrangement (e.g., single-layered) and the cell surface (e.g., by kinocilia in the respiratory epithelium).
General functions of epithelial tissue include a barrier (protection of tissues from radiation, desiccation, invasion by pathogens and toxins), secretion (substance release of hormones, sweat, mucus, and enzymes) and absorption (substance intake). It contains no blood vessels and no nerve supply; the “cell nourishment” takes place between individual epithelial cells through the intercellular space.
The epithelial tissue has a general characteristic that their cells are closely bound to each other through specialized structures such as tight junctions, desmosomes, interdigitations, gap junctions, and intercellular bridges. These gap junctions help in communication with two cells together by cementing each other. They constitute the linings of organs and body parts, they have one surface that is not attached to any cell, either exposed to the external environment or the lumen of an organ. They don’t possess blood vessels and their nutrients requirement is fulfilled by connective tissue forming the basement membrane.
The three characteristics of any epithelium. Image by Lecturio
Epithelial cellular organizations are located on the basal membrane. The basal membrane is a thin extracellular matrix. It consists of the basal lamina, which is itself divided into the laminae rara externa et interna, the lamina densa and the lamina fibroreticularis (except in renal corpuscles).
The function of the basal membrane is to stabilize the epithelial and endothelial cell layers. The attachment of cells is achieved with the help of syndecan or laminin and integrin. Microfilaments attach the lamina fibrorecticularis to the perlecan in the lamina densa. Epithelial cells regenerate on the basal membrane.
Electron microscopic image of the basal lamina
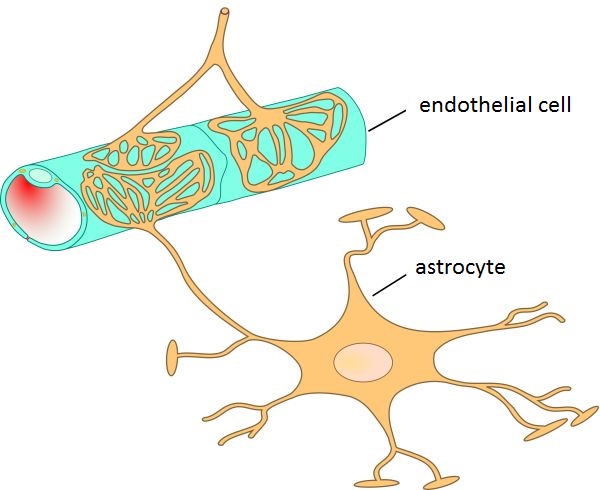
The surface epithelium primarily has barrier and transport functions. It is a mechanical and chemical barrier that prevents the uncontrolled substance exchange. It takes substances in (absorption) or releases them into the tissue (secretion).
Image: “Schematic representation of the endothelium with astrocytes in the blood-brain barrier” by Kuebi (added translation). License: CC BY 3.0
The simple epithelial tissue is a closed network of flat epithelial cells. These are located on the basal membrane. It is composed of a single layer of cells that are specialized in diffusion, osmosis, filtration, secretion, and absorption. The simple epithelial tissue is found in the alveolar epithelium (pulmonary alveolus), the endothelium (lining of blood vessels and lymph vessels) and the mesothelium (lining of the body cavities). Medically, the simple epithelium is further divided into two types: simple cuboidal epithelium and simple columnar epithelium.
The cells of the cuboidal epithelium are equally tall as they are wide and have a central round nucleus. The simple cuboidal epithelium is found, e.g., in kidney tubules and seminiferous tubules as well as in glandular excretory ducts and as retinal pigment epithelium and lens epithelium in the eye. They have large cytoplasmic content so, they perform important complex functions like absorption and secretion. They are found in exocrine glands, endocrine glands, and ducts of endocrine glands.
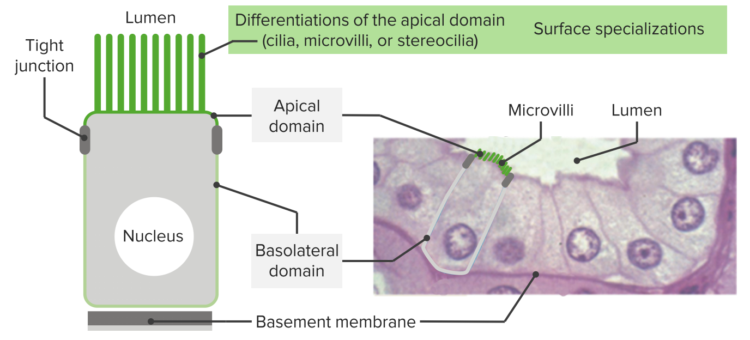
Electron microscopic image of human jejunum epithelium cells with densely packed microvilli.
The simple columnar epithelium consists of longitudinal-oval cells with a uniform nucleus, aligned in a row mostly located at the base of the cell. Their apical surface is often covered with microvilli to facilitate a strong absorption. This epithelium type can be found in high secretary areas and absorptive areas, for example, in the stomach, intestines, gallbladder, fallopian tubes and uterus.
The classification of stratified epithelium is based on the cell shape of the superficial layer. If, for example, the superficial layer consists of flat cells, it is part of stratified squamous epithelium. They are multilayered found in parts where protection from mechanical or chemical abuse is essential. The stratified epithelium is classified into three different forms.
The cell shape of the stratified, non-keratinized squamous epithelium changes from the basal toward the free surface and is divided into four sections:
- Stratum basale: prismatic dark-colored cells with a round nucleus
- Stratum parabasale: polygonal dark-colored cells arranged in stratified tissue
- Stratum spinosum: polyhedral, polygonal cells connected by desmosomes
- Stratum superficiale: flattened cells degraded and desquamated in the outermost layers
This type of epithelium is found in the mucosa of the oral cavity and esophagus, as well as the vagina and in the eye (corneal epithelium).
The outermost cell layers of the epithelium consist of flattened cells with no nuclei and cytoplasm, converting into scales. They are called stratum corneum, and their purpose is to mechanically protect underlying tissue from dehydration.
The stratified, keratinized squamous epithelium is divided into five sections:
- Stratum basale
- Stratum spinosum
- Stratum granulosum: flattened cells with keratohyalin granules
- Stratum lucidum: conversion area
- Stratum corneum
The above structure shows an example of the typical skin epithelium—the epidermis. It is the outermost layer of the three layers that make up the skin, the inner layers are the dermis and hypodermis.
Image: “Mucous membrane of urinary bladder with urothelium.” by Polarlys. License: CC BY-SA 3.0
The urothelium consists of a basal layer, several intermediate cells layers, and an umbrella cell layer. Umbrella cells (superficial cells) are large and often have two nuclei. The crusta, a very dense network of cytoplasm, is located beneath its apical membrane. The plasma membrane consists predominantly of rigid plaques containing uroplakin (transmembrane proteins). Transitional epithelium is primarily found in the efferent urinary tract, i.e., in the renal pelvis, ureter, urinary bladder and the initial part of the urethra.
The important characteristic of this epithelium type is that their cells do touch the basal membrane, but not all of them reach the free surface. The cells that reach the free surface belong to the columnar type. The cells that do not reach the free surface rest on the basal lamina and have a round nucleus. The term pseudostratified is derived from the appearance of this epithelium. Because the cell nuclei appear at different heights, it conveys the erroneous impression that there is more than one layer of cells. The non-ciliated pseudostratified epithelium is found, e.g., in the epidydimal duct and vas deferens, and ciliated pseudostratified epithelium with kinocilium is found in the respiratory tract (nasal cavity and bronchi).
| Cells | Location | Function |
Simple squamous epithelium | Air sacs of lungs; lining of the heart; blood vessels and lymphatic vessels | Allows materials to pass through by diffusion and filtration; secretes lubricating substance |
| Simple cubo /> | In ducts and secretory portions of glands; in kidney tubules | Secretes and absorbs |
Simple columnar epithelium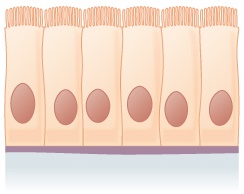 | Ciliated epithelium in the bronchi, fallopian tubes, and uterus; smooth (non-ciliated) epithelium in the digestive tract and urinary bladder | Absorbs; secretes mucous and enzymes |
Pseudostratified epithelium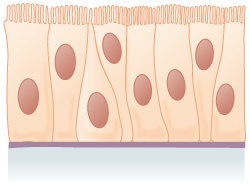 | Ciliated epithelium lines the trachea and a large part of the upper digestive tract | Secretes mucous, which is moved by ciliated epithelium |
Stratified squamous epithelium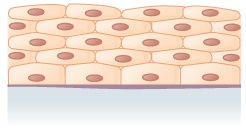 | Lines the esophagus, mouth, and vagina | Protects against abrasion |
| Stratified cubo /> | Sweat glands, salivary glands, mammary glands | Protects |
Stratified columnar epithelium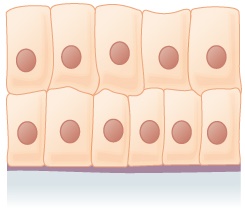 | Male urethra, some glandular ducts | Secretes and protects |
Transitional epithelium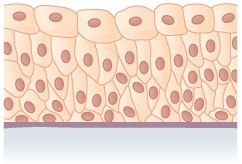 | Lines urinary bladder, urethra, and ureters | Allows the urinary tracts to stretch |
Images: “Summary of Epithelial Tissue Cells“ by Phil Schatz. License: CC BY 4.0
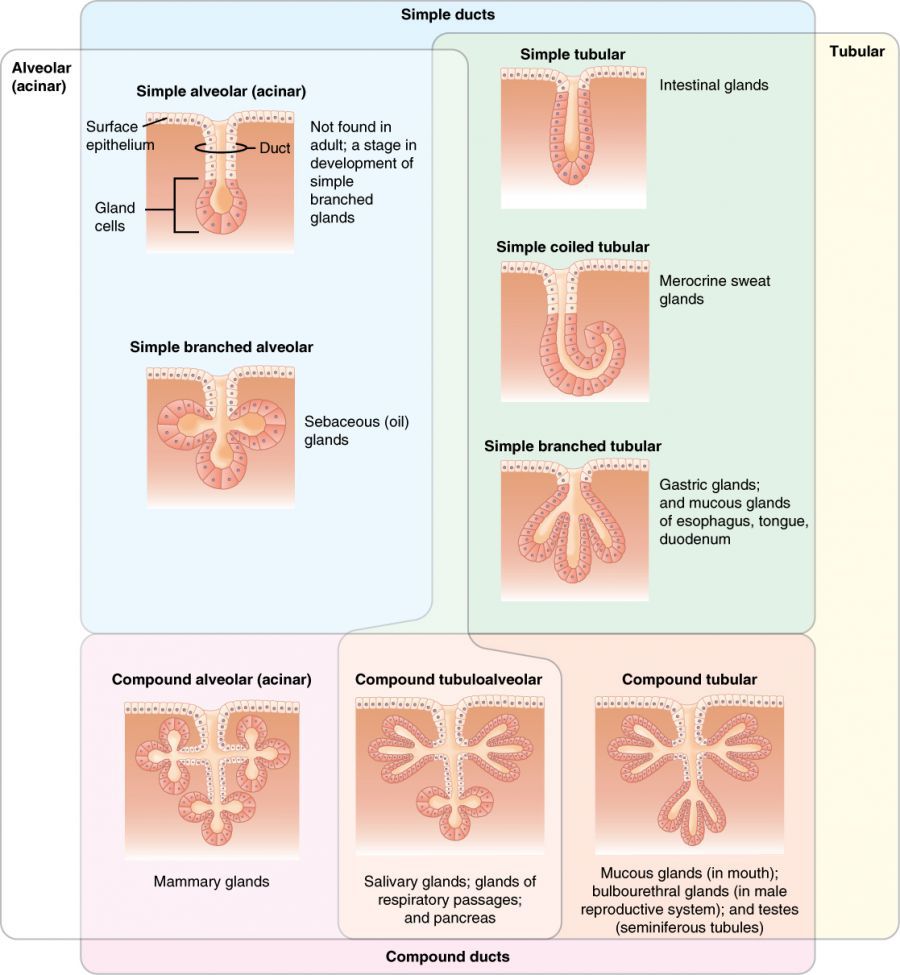
Associations of particularly differentiated and specialized epithelial cells are called glandular epithelium and consequently located in the glandular tissue. They have specialized in producing substances such as enzymes, hormones, sweat, oil, mucus, etc. and releasing them in the organism (secretion). The elaboration and release are carried out by external stimuli or constitutively into ducts on the surface or into the blood. Based on the specialization of the glandular epithelium, we distinguish between exocrine and endocrine glands. The classification is based, among other factors, on the number and location of secreting cells and the type of secretion.
Image: “Exocrine glands are classified by their structure.” by Phil Schatz. License: CC BY 4.0
Exocrine glands secrete their products through a duct onto the inner or outer surface of the body. They have their own ducts and extensive blood supply and are in control of hormones and nerves. Examples are salivary glands, sweat glands, tear glands and mammary glands of the breast.
Endocrine glands release their incretions directly into the bloodstream and therefore have no excretory duct. Incretions are mostly hormones. Examples of endocrine glands are the thyroid gland, as well as testicles and ovaries.
The pancreas has the particular anatomical and physiological characteristic of having both types of glands. Its exocrine portion passes digestive enzymes through the pancreatic duct into the duodenum, while the endocrine portion (islets of Langerhans) produces the hormones insulin and glucagon and releases them into the body.
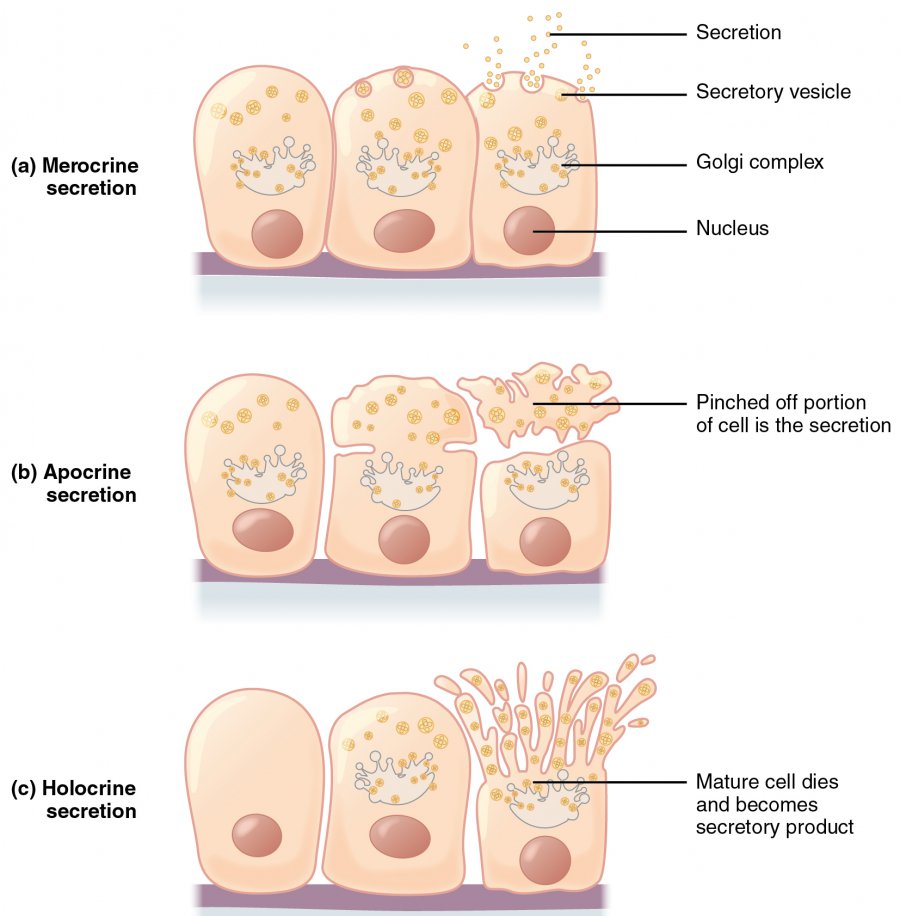
Image: “Modes of Glandular Secretion” by Phil Schatz. License: CC BY 4.0
In addition to the physiology and histology, a physician should know, understand and treat the pathology of the epithelium. Below you will see some examples of specific disease types and their symptoms.
In simple wounds, like cut, scrapes, the healing process is done by the proliferation and spread of epithelial cells in 24 hours. Deep burns (third degree) are largely corrected by epithelial regrowth.
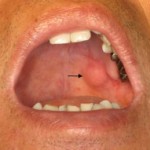
Image: “ Tumor located in left soft palate” by openi. License: CC BY 2.0
Papillomas are benign epithelial tumors. They grow instratified squamous epithelium. The most frequent form is the wart (basal cell papilloma), a proliferation of epithelial cells from the stratum basale of the skin. The result is a compact organized epithelial node that can keratinize.
Like the papillomas, adenomas are also benign epithelial tumors that can grow in glands. Adenomas can develop into malignant tumors, the so-called adenocarcinomas.
When in contact with a specific allergen, the skin epithelium is loosened up like a sponge by the formation of edema. This edema is an intercellular accumulation of fluid that can also converge into bubbles. Typical allergens that cause such eczema are, e.g., animal hair (epithelium allergy).
If an unusually high concentration of epithelial cells is found in urine or urine sediment samples, it should be assumed that a urinary tract infection has taken place. Its causes need to be clarified by further analysis.
Ichthyosis refers to various forms of mostly genetically determined skin keratinization. Patients suffer from large scaly hyperkeratosis of the skin with impaired desquamation.
Image: “Lamellar Ichthyosis with Rickets” by openi. License: CC BY 3.0
The answers can be found below the references.
1. Which of the following statements on the epithelial tissue is not correct?
- From an embryological perspective, epithelial tissue is derived from all three germ layers.
- Epithelial tissue has no significant intercellular substance.
- Epithelial tissue is found on the skin surface or on the internal surface of hollow organs.
- Epithelial tissue is supplied in intercellular spaces and through blood vessels.
- Epithelial cells have an apical and a basal pole.
2. How many types of single-layered (simple) epithelium are there?
3. Which of the following is not a part of the basal lamina of the basal membrane?
- Lamina rara externa
- Lamina densa
- Lamina propria
- Lamina fibroreticularis
- Lamina rara interna
источник